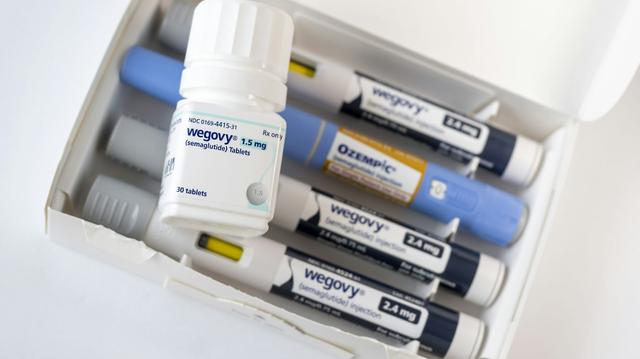
After years of success at Wigway, an Oakland patient is facing a setback as California cuts Medi-Cal coverage for long-term obesity drugs, putting his health at risk.
Michael Silk/Universal Pictures Group via Getty Images
I’ve lived with chronic obesity since I was 18 months old. For decades, it has shaped every part of my health and increased my risk for serious disease. Throughout my weight journey, I’ve followed guidance from doctors and public health experts, walking one to two miles a day, adhering to nutrition programs and staying disciplined. When that wasn’t enough, I turned to sleeve gastrectomy bariatric surgery at age 53 to save my health. Still, it wasn’t enough to maintain a consistent, healthy weight.
[–>
Having access to the new generation of weight-losing drugs has finally made the difference. They are known as GLP-1, or glucagon-like peptide-1 receptor agonists, with commercial names like Ozempic and Wegovy. For the first time since infancy, I’ve finally reached a healthy weight range. My blood pressure issues have subsided, and I no longer needed medication for them.
[–>
Now, I’m terrified all of that progress will be undone, and I’ll end up right back where I started. Not because the treatment failed, but because state leaders decided it was no longer worth covering under California’s Medi-Cal program for people living with chronic obesity.
[–>
Like the millions of others living with chronic obesity, I know the vicious cycle of short-term progress followed by inevitable regain. I needed a GLP-1 medication, and Medi-Cal made that treatment affordable. But this isn’t just my story. Nearly one in three adults in California lives with chronic obesity, and almost 15 million people rely on Medi-Cal.
[–>
At the start of this year, lawmakers cut Medi-Cal coverage for anti-obesity medications for people whose primary diagnosis is chronic obesity, recommending diet and exercise while ignoring that many of us have spent decades doing exactly that. Telling someone who has exhausted every option and undergone major surgery to simply “try harder” is not care. It is a weight-biased policy that ignores medical evidence about obesity’s causes and its treatment, and shifts blame onto the individual.
[–>
The reasoning makes it worse: With obesity no longer covered, my doctor requested prior authorization to continue GLP-1 treatment for obstructive sleep apnea, a condition the state said would still qualify. That request was denied because my numbers had improved. In other words, the treatment worked, and that success was used to justify taking it away.
[–>
What I’ve learned through this process is that obesity is treated differently from almost any other chronic disease, even though the National Institutes of Health and the American Medical Association recognized it as one. When other conditions improve, treatment continues to keep them stable. With obesity, getting better can mean losing care.
[–>
Obesity is not a moral failure, it’s biology. Yet people like me are still made to prove we deserve treatment.
[–>
The state claimed it needed to “cut costs.” But withholding treatment for chronic obesity just shifts expenses. Untreated obesity can lead to diabetes, heart disease, sleep apnea, kidney failure and disability — all of which would cost the state far more to treat than obesity itself.
[–>
Without Medi-Cal, there is no way I can afford Wegovy or any alternative on my own. I’ve researched my options. The truth is, there are none. Cutting coverage for this treatment will hurt the very people Medi-Cal was created to protect.
[–>
California says it leads with science and compassion. By cutting treatment for chronic obesity, it is doing the opposite. If lawmakers want better health and lower long-term costs, they should restore access to anti-obesity medications.
[–>
Shekinah Samaya-Thomas is an adult educator, citizen advocate and member of The Obesity Action Coalition. She lives with her husband in Oakland.
#Weight #loss #pills #saved #California #lawmakers #remove #opinion